Applied Behavior Analysis (ABA) 101
Applied Behavior Analysis (ABA) is a type of therapy that seeks to improve or teach specific behaviors in areas such as social skills, communication, self-care, and academics. It is most often used to support individuals with autism. So, what does ABA look like? How can you find a provider, and what is the best way to get ABA funded? We spoke with Faye Carter, PhD, BCBA-D, regional director of ABA services for STAR of CA, and Jennifer Symon, PhD, BCBA-D, a professor in the Division of Special Education at California State University, to get the details.
What does ABA therapy look like?
ABA looks at what happens immediately before, during, and after a behavior occurs in order to create an intervention plan. As Faye Carter explains, “It’s about: what are the triggers of this behavior? What are the consequences of this behavior? What’s a replacement for this behavior?” A therapist can use this data along with reinforcers to help a child work on skills like communication, adaptive behavior, language, and more.
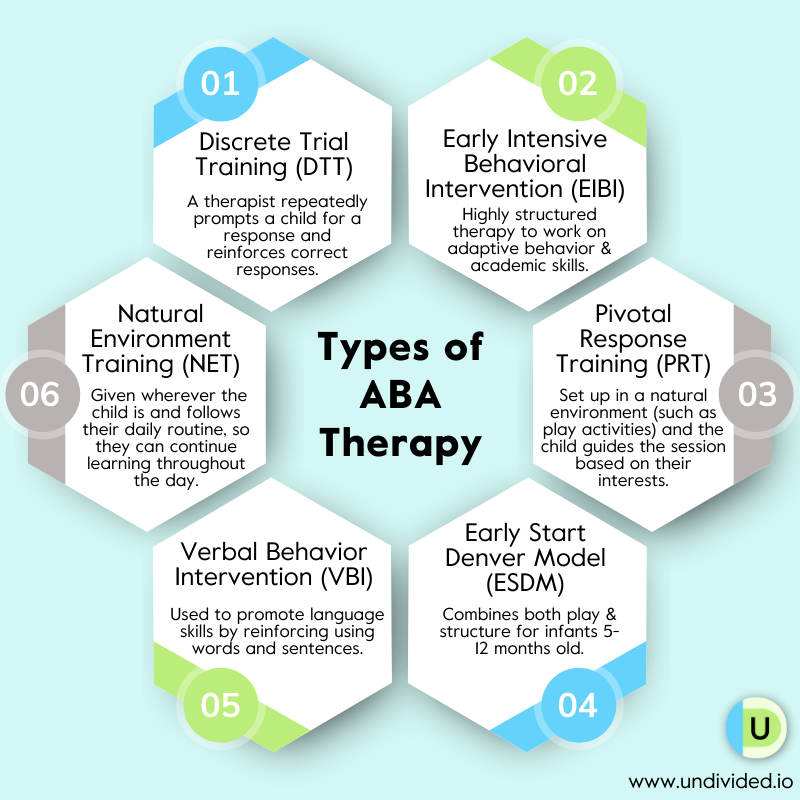
ABA is an umbrella term encompassing different methodologies. A therapist may use one or more of the following:
This is just a very brief overview of some of the types of ABA therapy. See our article on the different types of ABA for a rundown of how these therapies work and more details about what strategies a therapist may use during sessions.
Is ABA therapy right for my child?
As a parent, the most important question is whether ABA therapy will benefit your child. Of course, the answer will depend on your family and child’s individual needs. ABA has been used effectively in a variety of settings for children with varying diagnoses, including:
Autism. A 2006 study suggested that ABA was effective for children with autism in increasing adaptive functioning. “Naturalistic teaching utilizing ABA instructional methods has been shown to increase expressive language, communication, and play skills,” according to a study in 2009.
Down syndrome. When a behavior intervention plan relies primarily on reinforcement or is paired with positive behavior support plans, ABA has been shown to reduce “challenging behavior” in children with Down syndrome.
Prader-Willi syndrome. By teaching replacement behaviors, researchers were able to effectively eliminate self-injurious behavior in one case study.
Attention Deficit Hyperactivity Disorder (ADHD). Behavior therapy can teach children with ADHD to self-monitor and manage tasks.
Intellectual disability. ABA therapy has been shown to successfully teach communication as well as pre-academic and adaptive skills to children with intellectual disabilities.
“We often have students with specific learning disabilities, visual impairments, and orthopedic or health impairments. Often, we use behavioral intervention strategies to teach various skills,” Jennifer Symon tells us.
Behavior therapists have also used ABA therapy to support children who use wheelchairs, walkers, assistive technology, or ventilators. Practitioners can use ABA-based physical therapy to support children using wheelchairs to gain posture control as well as visual-motor skills to help them assess the distance between themselves and objects in their environment. In addition, research has shown that access to high-preference toys, used as reinforcers, can successfully decrease the rate of ventilation tube disconnection.
Criticisms of ABA
When ABA was being developed in the 1960s, it looked different than it does today, and these practices continue to be a concern for some parents. For example, during the first discrete trials, researchers would offer a reinforcer or reward for a correct response, but in some cases, children received unpleasant or painful stimuli such as electric shocks for incorrect answers. These stimuli, called “aversives,” are no longer widely used. The Professional and Ethical Compliance Code for Behavior Analysts states: “Behavior analysts recommend reinforcement rather than punishment whenever possible.”
Others worry about behavior control and whether ABA is used ethically. For example, during early research, researchers would use punishment to discourage a young boy from playing with traditionally feminine toys, such as dolls. Critics also question who gets to decide what a “problematic behavior” is. Some individuals with autism feel that their experience with ABA was “torturous” and an “attack on their identity,” and some have reported having symptoms of PTSD as a result.
It’s important to note that many of these experiences have been shared by adults who received ABA services as children, and they may not reflect modern practices. Currently, many consider ABA therapy to be the gold standard for supporting individuals with autism.
Symon adds, “I wouldn’t want to change everyone to be a certain way. At the same time, I want to allow people to learn the skills that they may not be learning on their own without some specific intensive support when they’re younger, so they can then decide what they want to do with their lives.”
Many behavior analysts have begun placing the focus on child preference and involvement to create positive, less aversive sessions. For example, Carter tells us that she likes to hold sessions that are play-based, “so it’s fun and exciting.” She says she makes sure to keep reinforcers highly motivating to keep children interested, so they are “not under duress” as they learn new skills.
Carter also tells us that the first few months of ABA can be stressful for children who are learning new skills that are hard for them. But, she says, “You try to intersperse eighty percent known and twenty percent new, so they can feel really successful and not overwhelmed.”
It’s important to create goals that are meaningful to the child and their family, and it’s essential that children are engaged in motivating activities. “We want to really bring their interest into the lessons, and that’s directly reinforcing them — versus they attend to the task we might want to present, and they earn reinforcement,” Symon says.
In a 2025 policy statement, the American Academy of Child and Adolescent Psychiatry (AACAP) said, “Physicians and other clinicians should consider a full range of evidence-based treatment options, not just ABA” so that children can get access to “timely, individualized care.” We cover plenty of examples of evidence-based, non-ABA therapies in our article about common behavior interventions.
How do I find an ABA provider?
There are multiple avenues available to parents when searching for a provider, such as requesting a list of in-network providers from your insurance company, or requesting recommendations from other organizations that specialize in supporting people with disabilities. Los Angeles Families for Effective Autism Treatment (LAFEAT) published a list of ABA providers in the Los Angeles area, and your local Autism Society of America chapter may be able to refer you to a provider. Depending on your state, disability organizations such as Regional Center in California may also be a resource for recommendations.
What should I ask a potential ABA provider?
Interviewing a potential provider is an important first step to see if they are a good fit for your child and family. Some questions you might ask include the following:
How many therapists do you put on a case?
What methodologies do you use? Do you only use Discrete Trial Training (DTT) or an array of ABA program types?
Do you meet the child where they are?
Are your goals and programs focused on skill-building rather than just compliance?
Do you ever use aversives in sessions?
What reinforcers do you use to motivate children during sessions?
- Some therapists may use food items as a reinforcer, which might not align with your child’s other goals, so it is a good idea to ask about the reward systems they have in place.
Do you provide support across multiple settings?
What does your parent training look like? How are parents included in the process?
What is your plan for children who aren’t making progress?
What process do you use when creating goals?
How many hours a week do you typically recommend?
- Carter tells us that some providers might suggest more hours than what is appropriate for your child. For example, if you have a two-year-old child, a forty-hour week may not be appropriate, as “you would be programming with them every waking moment that they are not eating or sleeping.”
If you're an Undivided member, click here for a printable checklist with these questions that you can bring with you to the appointment or have in front of you on the phone.
It can also be helpful to pay attention to whether or not the provider is asking you questions. For example, are they asking about the goals you have in mind for your child? As Symon says, “What have you always dreamt of doing with your kids, and how can we help them to do those things?” It is essential for goals to be individualized, meaningful, and valuable for your child and family.
Symon adds that the relationship between a child and their therapist is unique; it’s important that they and your child click. “You might get a therapist and a child, and they end up getting in their groove and clicking and getting along really well together. Then you also might have, even within the same agency, another person who is just not as good of a fit.” Parents should consider whether supervisors, therapists, and other staff have a good rapport with the child.
When considering potential ABA providers, it’s essential to ask yourself and your child, “Do you feel comfortable?”
Find an ABA provider
How can I fund ABA services for my child?
ABA services can be expensive when paid for out of pocket, so look first to these options:
Private insurance: Contact your plan’s member services department to see if your plan will cover behavioral health services. To receive coverage, your child will need a prescription from their doctor or psychologist who has determined that ABA is medically necessary. If you are denied coverage, you can submit an appeal through your member services department.
- In some states, like California, behavioral health services may be mandated coverage for commercial private insurance plans but not employer-based plans. Undivided’s Director of Health Plan Advocacy, Leslie Lobel, tells us that some families buy a secondary private individual plan just for their child to access ABA funding if their primary insurance is a self-insured plan.
Public insurance: Medicaid will cover behavioral health services under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit for beneficiaries under twenty-one years old. To receive coverage, your child will need a prescription from a doctor or psychologist who has determined that ABA is medically necessary. If ABA services are denied or changed and you disagree with the decision, you can request a fair hearing to appeal the decision.
- If your child has dual coverage, ABA services will be primarily funded through the private plan; however, Medicaid can be used to offset other costs, such as copayments.
Other public benefits programs: State agencies may be available to fund ABA therapy if you are denied services by your insurance. For example, Regional Center in California can fund as a payor of last resort and can also coordinate services and provide evaluations and assessments at no cost to those who are eligible.
Your child's school: If your child requires ABA to receive a free, appropriate public education (FAPE), the service can be written into your child’s IEP.
Request funding for my child's Applied Behavior Analysis (ABA) therapy
Resources
To learn more about ABA, you can visit:
- The Behavior Analyst Certification Board’s official website
- The Association for Behavior Analysis International’s Learning Center
- Components of a Quality ABA Program
Join for free
Save your favorite resources and access a custom Roadmap.
Get StartedAuthor